|
The Orthopaedic
Journal at Harvard Medical School is now an annual tradition in the
Harvard Combined Orthopaedic Residency Program. It has become an exceptional
way to celebrate the many successes among the entire staff and to give
readers the sense of community in our program. In particular, I ’m
pleased to give to you my third annual report and to reflect upon our
significant accomplishments at the Massachusetts General Hospital.
 |
| Dr.
Andrew Freiberg |
NEW
CLINICAL FACULTY
It is a great pleasure to welcome Dr. Andrew Freiberg, Assistant Professor
of Orthopaedics and Assistant Orthopaedic Surgeon back to the MGH. Dr.
Freiberg completed his Residency in Orthopaedic Surgery at the University
of Michigan and completed a Fellowship in Total Joint Arthroplasty at
the MGH. He returned to the University of Michigan Hospitals as the Chief
of the Adult Reconstruction Service and developed an outstanding Arthroplasty
Service and reputation in the field of total joint replacement. Dr. Freiberg
joined the MGOA in August 2000 and he is occupying the space vacated by
Dr. Don Pierce on ACC 537. Dr. Freiberg said of his return to the MGH,
“ I ’m delighted to be part of the Department of Orthopaedic
Surgery. I have been welcomed back into a progressive and talented group
of surgeons. As the newest member of the Adult Reconstructive Service,
I hope to continue a strong tradition of patient care, education and research.
”Dr. Freiberg plans to develop an active arthroplasty practice and
will be instrumental in helping us lead the Knee Biomechanics and Biomaterials
Laboratory. In addition, to his work in Arthroplasty, Dr. Freiberg has
a keen interest in gene therapy for Rheumatoid Arthritis. He has published
extensively in the area of adult arthroplasty and we welcome him to the
Arthroplasty Service. We also welcome his wife Dee and his children, Stephen
(age 9) and Benjamin (age 8) .
 |
| Dr.
Julie Katarincic |
It is also a great
pleasure to welcome Dr. Julie Katarincic as an instructor in Orthopaedics
and as an important new member of the Hand Service. Dr. Katarincic joined
us in November 2000 from the Mayo Clinic where she was actively involved
in pediatric and adult hand surgery and was an active participant in the
Mayo residency training program. Dr. Katarincic completed her Orthopaedic
Residency at Brown University and followed with a Fellowship in Hand and
Microvascular Surgery at the Mayo Clinic. She furthers the depth of the
Hand Service and joins an already outstanding group of clinicians. Dr.
Katarincic remarked, “ Our family has had a wonderful experience
being welcomed to the MGH and Boston communities. The Orthopaedic Department
has such a strong presence, full of talented individuals on all levels.
It is exciting to be a member of this group and I hope to contribute to
the continuing growth of the Department. ” In addition, she will
be working with the Pediatric Orthopaedic Service as well with the Shriners
Hospital. We welcome Dr. Katarincic to Boston with her husband, Dr. Chris
Breen, Fellow in the Sports Medicine Service as well as her two children,
Conor (age 3) and Courtney (age 1) .
 |
| Dr.
Andrew Hecht |
It is also with great
pleasure that we welcome Dr. Andrew Hecht back to the MGH. Dr. Hecht will
be joining the Spine Service in August, 2001. Dr. Hecht trained in the
Harvard Combined Orthopaedic Surger y Residency Program. He was an out-
standing Chief Resident at MGH and is completing a Spine Fellowship at
Emory University Spine Center in Atlanta. Dr. Hecht ’s areas of clinical
interest include cervical spine surgery and spine trauma. His research
interests are in the areas of the biology of the invertebral disc and
the pathophysiology of disc degeneration. Dr. Hecht will be an integral
part of the expanding MGH Orthopaedic Spine Center. We welcome Dr. Hecht
to Boston with his wife, Dr. Sonia Nagy Hecht, an Infectious Disease Specialist
who will be joining the staff of the Beth Israel/Deaconess Medical Center
as an HIV Specialist. In addition, to these latest members of the MGH
Orthopaedics team we are actively recruiting a new Pediatric Orthopaedic
Surgeon. Also, we hope to have a new member of the Partners Trauma Service
in the near future.
ADMINISTRATION
In 1999 we welcomed
David Gaynor, our new Administrative Director of the Orthopaedic Service.
Mr. Gaynor has been an outstanding asset to the practice and plays a pivotal
role in implementing changes to improve efficiencies in the Department.
He is working on assembling an increasingly outstanding administrative
team to help him with these many functions and the heavy demands of our
increasing admissions, surgeries, and visits. Mr. Gaynor is actively involved
in the planning and strategic development of the MGH Orthopaedic website,
which will be undergoing renovation in the coming months. Mr. Gaynor reports,
“ we have recently begun a project to overhaul the Department website
in accordance to changes with the MGH main site and will be instituting
new plans and formulas directed at advancing the use of the site both
within the MGH community and outside. ”Mr. Gaynor has been instrumental
in reorganizing the Trauma Practice in the Ambulatory Care Building, and
making the many neces- sary moves to accommodate our new practitioners.
He ’s a thoughtful, insightful individual who ads great depth to
the Department and its administrative activities. Mr. Gaynor commented
on his time here, “ the Department of Orthopaedics has experienced
significant growth and development over the last two years. It is an exciting
process to watch the expansions and reorganizations that have been the
hallmark of success within the Department. I feel fortunate to be a part
of this organization and I look for ward to a long tenure here. ”
In addition, Mr. Gaynor has been an instrumental voice, along with myself,
in the planning and development of a new Ambulatory Care Center, which
I will discuss later in this report. I look for ward to Mr. Gaynor ’s
many significant contributions to our Department.
The administration
team has seen some additional chang- es with the recent retirement of
Rosalie Martin, Administrative Director for Finance. Her wonderful personality
and tremen- dous experience will be sorely missed. We are pleased though,
that we will benefit from her expertise on occasional special projects.
This year we welcomed
Karen M. Bernstein, Clinical Research Editor, to the Department. Ms. Bernstein
came to us after seven years with the Science and Publications Department
of the American Society of Clinical Oncology (ASCO) . Ms. Bernstein will
be dividing her time between supporting the editorial side of my research
work and serving as the content editor, developer and author of the Department
’s new web page. I am pleased to have Ms. Bernstein onboard in the
department and as a ringer on my team for the Annual Harvard Golf Outing.
AMBULATORY
CARE BUILDING
 |
| MGH
The New Millenium |
The Partners Finance
Committee recently approved two new buildings to be added to the Massachusetts
General Hospital. One will be a new Cancer Center near Cambridge Street
and the other a 200, 000 square foot new Ambulatory Care Building over
the Proton Beam Area. These two new buildings which are being constructed
over the next three years will add immensely to the clinical activities
of the institution. The Orthopaedic Department will be a proud occupant
in the new Ambulatory Care Building and will most likely occupy two floors
and 44, 000 square feet with the opening of a new MusculoSkeletal Institute.
We anticipate new practice modules with centralized radiology services,
as well as expanded wait- ing areas, minor procedure rooms, and new offices
for our practitioners. A massive fund-raising activity is underway to
raise 90 million dollars of philanthropy toward this project. I feel that
the new building combined with our outstanding commitment to patient care
will make the new MGH building second to none. In addition, this facility
will give us an opportunity to co-locate with other services that deal
with the same patient population and to develop a closer relationship
with Rheumatology, Physical Medicine and Rehabilitation, Pediatrics, and
Women ’s Health. It will also give us an opportunity to obtain new
economies, and to co-locate with important functions in Radiology. The
new ambulatory build- ing will provide an exciting opportunity to consolidate
the MGH Orthopaedics Department in one location enabling us to provide
high quality orthopaedic services more efficiently and effectively. Mr.
Gaynor, Dr. Andrew Freiberg and the administrative staff have been instrumental
in the coordination of the many activities in the new building.
NEW
PRACTICE MODEL
At this point
our new practice model has been fully insti- tuted. We now utilize combined
surgical and test scheduling, academic support services, nurse practitioners
and physician ’s assistants to improve our overall efficiencies and
patient satisfaction.
The Massachusetts
General Hospital Orthopaedic Associates (MGOA) now has control over our
complete revenue cycle. Tom Amerault, the new Director of the Orthopaedic
Billing Office has created an outstanding billing office with personnel
deployed in the appropriate billing areas. In addition, we will be hiring
a new billing liaison to work with high-volume practices in the group.
Mr. Amerault reports, “ through the collaborative efforts of the
whole Department, reimbursement will be maximized. ”The billing office
has officially moved to its new location and I am hopeful that we will
benefit from the new deployment of the IDX System at the MGH.
Our clinical and surgical
activities continue to grow. We have greatly increased our capacity for
patients in all practice MGH New Millenium 30 locations and have been
able to incorporate the new physicians into our relatively tight clinical
areas. Dr. Mark Vrahas, the new Partner ’s Chief of Orthopaedic Trauma
and Lillian Figueroa, have reorganized the Trauma activities in the ACC
525 area. Dr. George Theodore has moved the Foot and Ankle Service to
Dr. Robert Boyd ’s former office at ACC 503. This expanded space
will accommodate new administrative and research functions for the Foot
and Ankle Service and provide space for Dr. James Heckman, the new editor
of the Journal of Bone and Joint Surgery (JBJS) , in the Foot and Ankle
Service area.
NEWS
FROM THE OPERATING ROOM
Major strides
have been made in the operating rooms at the MGH over the past year. We
have fully implemented a new Orthopaedic Trauma Room. In addition, through
the efforts of the Operating Room Operations Improvement Committee, we
hired a new nurse manager for the Orthopaedic Service, and have also hired
an additional equipment manager. Furthermore, we have also acquired much
needed additional time in the main OR and in the same day unit. Additionally,
we have ordered over $350, 000 worth of equipment this year ($850, 000
over the past 3 years) to further facilitate our on time case starts,
decrease our turnover, and to upgrade and improve our equipment status.
In the near future we will be expanding the length of the operating room
day for Orthopaedic Operating Rooms, and adding additional rooms in the
same day unit. I would like to thank Drs. J. P. Warner, Bill Thomford,
and Mr. David Gaynor for their outstanding contributions.
SERVICE
UPDATES
ADULT RECONSTRUCTIVE
SURGERY SERVICE
The Adult Reconstructive
Surgery Service at the MGH led by Dr. William Harris is our most active
inpatient division within the department. With the addition of Dr. Andrew
Freiberg we expect further growth in the clinical area. Dr. Freiberg ’s
focus on revision total joint arthroplasty and his keen interest in knee
arthroplasty will add needed depth to the service. Dr. Harris agrees,
“ This has been a particularly eventful year for the Adult Reconstructive
Service. The return of Andy Freiberg to the staff strengthened and enriched
our facility. ”The renowned Harris Hip Course and the Harvard Knee
Course continue to highlight CME activities on the Adult Reconstructive
Surgery Service. My own practice continues to grow and I look for ward
to further clinical activity.
The introduction of
electron beam cross-linked polyethet- hylene to the marketplace has begun
a new revolution in total joint arthroplasty. With its extremely low-wear
characteristics it offers new opportunities in the area of total hip arthroplasty
with expanded head size and joint stability. The cross-linked polyethethylene
may permit new opportunities in primary and revision total knee arthroplasty
and unicompartmental arthroplasty. Dr. Harris said, “ on the research
front the singular event was FDA approval of the electron beam cross-
linked polyethylene for use in total knee replacement surgery. ”
This compound is being looked at in a variety of other joints throughout
the body and will be opening remarkable vistas for total joint replacement
surgery. Congratulations to Dr. William Harris and his team for this most
important contribution. It is a pleasure to announce that Dr. Harris was
recently honored as the recipient of the Maurice Muller Award. He traveled
to Switzerland to receive this highly coveted citation.
Fundraising efforts
have begun to endow the first Hugh P. Chandler Adult Reconstructive Fellowship
at the MGH. I am pleased to announce that we are well on our way to making
this a lasting contribution to the Adult Reconstructive Surgery Service
at the MGH. Dr. Chandler continues to improve and is spending a great
deal of time traveling and sailing.
 |
| Dr.
William Maloney and Dr. Harry E. Rubash |
WILLIAM
H. HARRIS FESTSCHRIFT CELEBRATION
In May, The Partner ’s Department of Orthopaedic Surgery and the
MGH hosted a Festschrift celebrating the achievements of an extraordinary
surgeon, teacher, and scientist, Dr. William H. Harris. Translated from
the German, fest means celebration and schrift means writing . A festschrift
celebration is a series of presentations and a volume of writings by different
authors bestowed as a tribute -especially to a scholar. The program participants
included former students of Dr. Harris and col- leagues who truly comprised
an intercontinental “ who ’s who ” of experts in joint
reconstruction. We were privileged to see an extraordinary array of scientific
presentations which spoke to the depth and breadth of the research and
clinical achieve- ments of Dr. Harris. We look for ward to the publication
of the Proceedings of the Scientific Event that will appear as a Supplement
to the Journal of Arthroplasty. In addition, this event also inaugurated
the William H. Harris Annual Lectureship. The lectureship will cover important
develop- ments in orthopaedic surgery and arthroplasty. We were pleased
this year to have Dr. William Maloney, Charles F. and Joanne Knight Distinguished
Professor at Washington University and Chief of the Orthopaedic Surgery
Service at Barnes-Jewish Hospital, as the first presenter of The William
H. Harris Lecture, with his talk on, “ Cartilage Repair Using Tissue
Engineering and Gene Therapeutic Techniques. ”
The culmination of
this special event was marked by the establishment of the William H. and
Johanna A. Harris Chair in Orthopaedic Surgery. This crowning achievement
is demonstrative of the wide impact Dr. Harris ’career has had on
Orthopaedic Surgery. The William H. and Johanna A. Harris Chair in Orthopaedic
Surgery will serve as a testa- ment to Dr. Harris ’commitment to
education, and research. Congratulations to Dr. Harris on this fine legacy.
Dr. Sam Thier, CEO and Chairman of Partners HealthCare System announced
Dr. James H. Herndon, Chief of Partners Orthopaedics, as the first recipient
of this esteemed position. As the inaugural recipient of The William H.
and Johanna A. Harris Chair in Orthopaedic Surgery, I am certain that
Dr. Herndon ’s tenure will mark a long tradi- tion of excellence
and accom- plishments here in the Harvard Orthopaedic Program. “
It is a real honor to hold the Chair of a man with such a dis- tinguished
record of contri- butions to orthopaedics and reconstructive hip surgery.
Dr. Harris was one of my teachers and it is especially rewarding, to be
given a Chair in his name, ”said Dr. Herndon. In 32 addition, we
are delighted to announce that Alan Gerry has generously established the
Alan Gerry Scholarship fund, equal to that of a Chair at Harvard Medical
School.
FOOT
AND ANKLE SERVICE
Under the direction
of Dr. George Theodore the Foot and Ankle Service on ACC 5 has experienced
exceptional clinical growth in the past year. The Service continues to
be at the forefront for treating cartilage injuries to the ankle and foot.
There have also been contributions in the area of post- traumatic reconstructions,
including fusions and osteotomies. Dr. Theodore reports, “ the Foot
and Ankle Service is dedicated to the development of innovative and minimally
invasive tech- niques for the treatment of adult foot-ankle problems.
Our cur- rent treatment emphasis is on cartilage injuries, arthroscopic
surgery, tendon reconstructions, and osteotomies. ”Recent research
activities include a study on shock-wave therapy for plantar fasciitis,
which moved from clinical trial to clinical use this spring. The Service
is looking for ward to the addition of a Fellow, and a new attending,
in the near future. Close collaboration with the Podiatry Service is also
underway.
PODIATRIC
UNIT
The Podiatric
Unit at MGH is nationally recognized for clinical care and post-graduate
education. As Director of Podiatric Medical Education, Dr. Robert J. Scardina
is planning development of an additional Residency Training year (PGY
III) , which would collectively lead to Board qualification for MGH graduates
in all three Podiatric sub-specialties (primary medicine, orthopedics
and surgery) .
The MGH Podiatric
Unit and MGH Podiatric Associates, emphasize a continuum of foot care
with attention to quality, cost efficiency, high clinical volume and state-of
–the-art treat- ment. Dr. Scardina reports, “ MGH Podiatry has
made remark- able progress in patient care and post-graduate education
and training. Additional Orthopaedic Department and Hospital support will
predictably lead to further growth, development and refinement within
all areas of our practice. ”The Podiatric Unit has realized growth
in outpatient volume by over 10% throughout the last year, with additional
access to services at the Main Campus as well as all three affiliated
Health Centers practices. Dr. Scardina and the entire Podiatric Unit staff
should be congratulated for recently achieving an additional five-year
approval status for the Residency Program(s) , as a result of a successful
Council on Podiatric Medical Education site visit. The Podiatric Unit
has worked closely with the Orthopaedic Department for over two decades.
HAND
SERVICE
The Hand Service
led by Dr. Jesse Jupiter continues to be the busiest service in the outpatient
unit at the MGH and has seen a great increase in the number of patients
treated. The Service has been greatly expanded by the additions of Dr.
David Ring, and Dr. Julie Katarincic. Dr. Ring who we welcomed last year
has a burgeoning practice. They both will continue to strengthen the ties
with the Trauma Service and the Pediatric Orthopaedic Service and will
greatly broaden the research interests in the unit including expanding
the area of microsurgical reconstruction. Dr. Jupiter reports that, “
our Hand Service has achieved an international reputation as a center
of excellence for the care of problems involving the upper limb. In particular
we are a renown center for the reconstruction posttraumatic problems of
the wrist and elbow and of microsurgical reconstruction of the extremities.
”The important AO Foundation Grant has recently been renewed and
is being used to develop a Center of Excellence for Hand and Upper Limb
Trauma and Reconstructive Problems at the MGH. Renovations of the Hand
Service clinical area are underway on ACC 5. 33
SHOULDER
SERVICE
The Partners
Shoulder Service is lead by Dr. Jon J. P. Warner and is housed at the
Physicians Office Building. This Service continues to grow exponentially
with over 500 shoulder surgeries being performed annually. In addition
to prolific clinical activities, over 4, 000 patients are seen by the
Service per year, Dr. Warner is running a first rate shoulder laboratory
concentrating on the area of shoulder stability. A strategic recruitment
is underway to further expand the clinical activi- ties of the Shoulder
Service. Dr. Warner reports, “ the growth in Clinical volume and
academic productivity has been very exciting over the past year. An additional
surgeon will soon join this service to expand our ability to meet our
goals of clinical excellence and academic advancement. ”
A number of prospective
clinical outcome studies have been initiated and collaborative research
projects continue with departments including Physical Therapy, Radiology
and Anesthesia. The Service ’s education programs also continue to
thrive. More than 20 foreign physicians have visited as Traveling Fellows
to the Harvard Shoulder Service. In addition, the Intercontinental Shoulder
Fellowship Program in collaboration with the University of Zurich has
become one of the most sought after Post-Graduate Fellowships in the world.
ONCOLOGY
It is a pleasure
to announce that the Orthopaedic Oncology Service at the MGH is under
the new leadership of Dr. Francis Hornicek. Dr. Hornicek reports, “
the Orthopaedic Oncology Unit is one of the busiest in the country if
not the world. With the leadership over the years of Dr. Mankin the Service
has reached its current outstanding reputation. Dr. Mankin, Dr. Gebhardt,
and I trust that this tradition will continue in the future. ”
Dr. Hornicek ’s
outstanding clinical expertise and his many contributions to the Orthopaedic
Training Program and Fellowship are greatly appreciated. The Service continues
its involvement in CME courses of Pathophysiology of Orthopaedic Disease
and the publication of numerous clinical and research reviews. The Connective
Tissue Oncology Clinic (CTOC) works closely with medical and radiation
oncologists, radiologists, bone pathologists and other integral medical
personnel and services to provide the most optimum care for patients.
Dr. Mark Gebhardt, President of the Musculoskeletal Tumor Society, whose
base has been at Children ’s Hospital, is spend- ing more time at
the MGH to help with the pediatric tumor cases. Dr. Gebhardt has been
an outstanding member of the service and we greatly appreciate his many
contributions to the Residency Program. I look for ward to Dr. Hornicek
’s many contributions to the area of musculoskeletal neurology
PEDIATRIC
ORTHOPAEDIC SERVICE
MGH recently
celebrated the opening of the new Massachusetts General Hospital for Children.
With the estab- lishment of this new hospital within a hospital, the Pediatric
Orthopaedic Service will be called upon to provide further leadership
in the expanding area of pediatric care at the MGH. Dr. David Zaleske
reports, “ the formation of the Mass General Hospital for Children
has been a wonderful event this year. This crystallizes our many activities
for children at the MGH. Dr. Alan Ezekowitz, Chief of
 |
| Dr.
Henry Mankin and Dr. Keith mankin |
Pediatrics, and Dr.
Rubash work even closer and the children benefit. The MGH Pediatric Orthopaedic
Service is undergoing an adolescent growth spurt. ”The Hospital is
giving a name to and reaf- firming what has always been a commitment to
outstanding service and care. This unique setting will serve as a bridge
to even further connect services in the area of pediatric care. The Pediatric
Orthopaedic Service continues to increase its role with the MGH Health
Centers and to further collaborations with the Boston Shriners Hospital
for children. It ’s great to have Dr. Zaleske expanding his clinical
practice.
We wish Dr. Keith
Mankin the best in his new home in the Raleigh-Durham area. Dr. Keith
Mankin decided to leave the MGH in January of 2001 and pursue a private
pediatric orthopaedic practice in North Carolina. Dr. Keith Mankin ’s
pediatric practice had grown tremendously over the past couple of years
and he will be greatly missed. We anticipate having a new faculty member
onboard by the summer of 2001.
SPORTS
MEDICINE
The Sports Medicine
Service at MGH continues to grow and prosper both in the clinical as well
as the research realm. The program is under the skillful leadership of
Dr. Bert Zarins, who has a long-standing history as a leader in the area
of sports medicine. In addition to an association with the New England
Patriots Football organization, the Boston Bruins, and the New England
Revolution Soccer team, the service is now participating in the care of
the new professional woman ’s soccer league team, the Boston Breakers.
The Service provides care for many local collegiate and high school athletic
programs. Reports Dr. Zarins, “ the MGH Sports Medicine Ser vice
provides evaluation, treatment, and rehabilitation of injured athletes
who participate at all levels of activity: recreational, amateur, professional
and elite. Our physicians provide medical care for four professional sports
teams, two colleges and two high schools. Our main research activities
include biomechanics of the post cruciate ligament, muscle injuries and
photodynamic therapy. ”Dr. Tom Gill through Dr. Henry Mankin and
Dr. Keith Mankin 34 a grant from the National Football League Charities,
is actively pursuing his research interests on posterior cruciate ligament
reconstruction with Dr. Guoan Li in the Robotic Joint Kinematics Laboratory.
Dr. Gill also has a CIMIT Grant for biological meniscus repair. Dr. Dinesh
Patel continues to excel in the area of arthroscopic learning programs
for our residents and fellows. A recent learning center program for the
Residents and Fellows was a wonderful success. The Sports Medicine Fellowship
is an outstanding one and has recently increased in its size.
SPINE
CENTER
The MGH Orthopaedic
Spine Center is now in its second year of existence. Drs. Frank Pedlow,
Fred Mansfield, and our new edition, James Sarni, staff the multidisciplinary
Spine Center. The Center is committed to offering timely evaluations and
highly organized treatment protocols for all spinal disorders. In terms
of clinical research the Service is working to develop and evaluate materials
and designs for prosthetic and lumbar disc replacement. The Service is
also involved in studies concerning spine reconstruction and fusion promotion.
In addition, Dr. Guoan Li and the new Robotic Joint Kinematics Laboratory
is collaborating with the Spine Center to further understand the biomechanics
of the spine. We are anxiously awaiting the arrival of Dr. Andrew Hecht
who will join the Spine Service in August 2001. The Spine Service is one
of the busiest in New England and also serves as an international referral
center for tumors of the spine and complex spinal reconstructions.
TRAUMA
SERVICE
 |
| Dr.
Malcom Smith |
The Partners Orthopaedic
Trauma Service under the skill- ful direction of Dr. Mark Vrahas has been
a continuing success at the MGH. Dr. Vrahas reports that, “ support
for the Trauma program from MGH, BWH and Partners affiliate hospitals
has been outstanding. ”Through an extensive outreach pro- gram, the
Service has positioned itself as the premier trauma service in the New
England area. Dr. Malcolm Smith, a Consultant Surgeon, from the Department
of Trauma and Orthopaedic Surgery at St. James ’ University Hospital
in Leeds, UK will be joining the Partners Trauma Service in August of
2001. It is a distinct pleasure to welcome Dr. Smith to the Partners Trauma
Service. He brings additional expertise and experience in the treatment
of patients of orthopae- dic trauma. Dr. Vrahas agrees, “ with the
addition of further staff this year we are on line to become a premier
center for the care of orthopaedic trau- ma. ”The Trauma Service
recently initiated a research study on the efficacy of autograft versus
a bone substitute for closed tibio- plateau fractures. In addition there
has been recent grant activ- ity with projects on “ The Relationship
between Chondrocyte Apoptosis and Post –Traumatic Arthritis in Humans,
”and “ Transitional Research Gene Therapy for Fracture Healing
– Bench to Clinic. ”The volume of this Service continues to
grow and the Chief Residents should be congratulated for their considerable
efforts. The Trauma Service Morning Report has been a great success and
we are pleased to announce that the Trauma Service recently won a Partners
in Excellence Award for their integrated efforts with Spaulding Rehabilitation
Hospital. In addition, the Partners Trauma Service recently received their
American College of Surgeons Level I Adult and Pediatric Trauma Accreditation.
RESEARCH
UPDATES
The faculty
and staff of the research laboratories have begun a reorganization of
the MGH Orthopaedic Research Laboratories. Dr. Orhun Muratoglu has been
assigned Chair of the new Executive Committee on Orthopaedic Research.
Dr. Muratoglu along with committee members, Drs. Francis Hornicek and
Teresa Morales, will be dealing with all laboratory activities. One of
the first charges I have given the Committee is to develop a template
and a working five-year plan document for all of the Orthopaedic Research
Laboratories at the MGH. In addition, this new Committee will be instrumental
in the allocation of the new research space that will soon be available
on Jackson 12.
Once again the scientists
of the various laboratories were extremely well represented at the Orthopaedic
Research Society (ORS) , with 20 podium and 28 poster presentations. Dr.
Stephen Trippel, the 2001 ORS Chairman and I, ORS Treasurer, have been
quite active on the Society ’s Board. I look for ward to further
participation from other members from our laboratories in the ORS. The
monthly MGH Laboratory Lecture Series has been an outstanding success.
Recent speakers have included, Drs. Gordana Vunjak-Novakovic, Stephen
B. Trippel, Julie Glowacki and Karen E. Yates. The Series has moved from
the Clinic ’s Amphitheatre to the recently renovated Ether Dome Amphitheatre.
In addition, we are able to watch the progress of a new mural documenting
the first public demonstration of anesthesia during surgery, which took
place in 1846 at the MGH. The Ether Dome Mural Project is being painted
by renowned Boston artist, Warren Prosperi and depicts a histori- cally
authentic rendition of the scene of the first application of ether. It
is fascinating to watch a great artist at work and we look for ward to
the official unveiling ceremony on Ether Day 2001.
Dr. Chris Evans has
been instrumental in the development of the new Center for Molecular Orthopaedics
in the Partners Orthopaedics Department. Dr. Evans reports, “ The
Center for Molecular Orthopaedics aims to develop molecular solutions
to orthopaedic problems. Gene therapy is the major, but not exclusive,
area of interest. During its first year of existence, the CMO has established
and staffed a laboratory in the Lying In building on Longwood Avenue.
In the coming year, it is hoped to establish a similar presence at MGH.
Together, these two laboratories will facilitate the translation of bench
research into novel clinical interven- tions. ”We will be hiring
a new molecular biologist that will work with the CMO laboratories in
new MGH Jackson Dr. Malcom Smith 35 12 research space. I ’m hoping
that this new individual will collaborate closely with the clinicians
in the MGH to explore this highly important and exciting new area of molecular
orthopaedics. Dr. Evans is an extremely productive individual is flourishing
in the Boston research environment. We all look for ward to the many contributions
from the Center for Molecular Orthopaedics.
ORTHOPAEDICS
BIOMECHANICS AND BIOMATERIALS LABORATORY
The Orthopaedics
Biomechanics and Biomaterials Laboratory is under the direction of Dr.
William Harris. This laboratory has developed numerous significant contributions
to the world of total joint arthroplasty. The Laboratory has been responsible
for clinical contributions in the area of cement technique, instrumentation
for total joint replacement, total hip and total knee implant design,
and a new electron beam cross-linked polyethylene (Longevity TM Zimmer,
Inc. , Warsaw Indiana) , Durasul TM Sulzer Orthopedics, Austin Texas)
, that most likely will revolutionize the area of total hip arthroplasty.
This laboratory has collaborated closely with other laboratories within
the institution as well as the Massachusetts Institute of Technology (MIT)
. Currently, the newly developed polyethylene is being used in total hip
arthroplasty and it has been approved for total knee replacement. It is
our hope that the new polyethelyenes will be available for other joint
arthroplasty sites. In addition, a very active program is underway looking
at osteogenic substances and their ability to repair osteo-defects. The
many contributions of Dr. Orhun Muratoglu, Chair of the Executive Committee
on Orthopaedic Research, Dr. Murali Jasty, Dr. Dan Estok, Danny O ’Connor,
Charlie Bragdon, Edie Weinberg, and many others have made this laboratory
one of the premier Biomechanics and Biomaterials Laboratory in the country.
Dr. Harris said, “ we also greatly benefited from the presence of
Henrik Malchau from Goteborg, Sweden as a Visiting Research Scientist
for the year, contributing to our rapid development in RSA. ”In addition,
he reports, “ we have also launched an electronic relational, Intranet
Database for gathering data for outcomes studies. ”The laboratory
was well represented at the ORS and we anticipate further significant
contributions.
BIOMATERIALS
RESEARCH LABORATORY
The Biomaterials
Research Laboratory located on Jackson 11 is under the direction of Dr.
Arun Shanbhag. This Laboratory utilizes a multi-disciplinary approach
to investigate complex orthopaedic biomaterials questions, and is focusing
on comprehensive investigations of periprosthetic osteolysis using the
newest cellular and molecular biological techniques. A grant to study
the genetic markers for arthritis was recently received. In addition,
the Laboratory has also received a NIH- RO3 Grant to study the anabolic
effects of bisphosphonates. This Laboratory will continue to provide unique
opportu- nities for scientists, residents, fellows and staff and is an
integral part of the future of Orthopaedic Research at MGH. Dr. Gun Il
Im, Mark Neavyn, Laboratory Technician, Sheeraz Qureshi, Jean-Pierre Phancaso,
and Mara Meyer, should all be recognized for their dedication and many
contributions. A congratulation goes to Arun Shanbhag who recently was
accepted to Boston University ’s intensive Executive MBA Program.
In addition congratulations to the Laboratory team for their well received
ORS papers and presentations.
KNEE
BIOMECHANICS AND BIOMATERIALS LABORATORY
The Knee Biomechanics
and Biomaterials Laboratory is another integral part of the Orthopaedic
Biomechanics and Biomaterials Laboratories at the MGH. The Laboratory
is now located on Jackson 11 and is continuing to study component wear
after total knee arthroplasty and the effects of component alignment on
implant wear. The Laboratory utilizes a multi-disciplinary approach including
finite element analysis, computerized modeling, and knee-wear simulators.
Investigators in this Laboratory are studying the complex interactions
between the tibiofemoral joint, the patellofemoral joint, and the effects
of alignment and rotation on knee function and wear. This Laboratory is
under the direction of Dr. William Harris and myself and draws upon the
expertise of numerous members of the Orthopaedics Biomechanics and Biomaterials
Laboratory. In addition the laboratory works closely with the Joint Kinematics
Laboratory directed by Dr. Guoan Li.
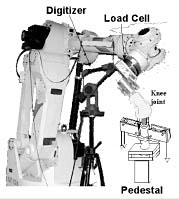 |
| Robotic
Joint Simulator |
JOINT
KINEMATICS LABORATORY
The new Joint
Kinematics Laboratory is under the direc- tion Dr. Guoan Li. Dr. Li and
his fellow scientists interact closely with clinicians in the Orthopaedics
Department. This Laboratory uses a sophisticated robotic joint simulator
to understand complex kinematics and biomechanics of the mus- culoskeletal
system. This Laboratory has important subdivi- sions, which include the
Hand and Upper Extremity Module, the Athletic Reconstruction Module, the
Total Knee Arthroplasty Module, and a newly developed Spinal Mechanics
Module. Dr. Li explains, “ The Joint Kinematics Laboratory utilizes
the most recent technological advances to delineate the joint function.
We are interested in the biomechanical factors that lead to joint Robotic
joint simulator 36 injuries and long-term joint degeneration. We also
examine the biomechanical effects of current surgical options used to
treat these injuries and devise new techniques. ”Congratulations
to Dr. Li on his podium and poster presentations this year at the ORS
as well as on his recent OREF Grant in collaboration with Dr. Tom Gill
to investigate the effect of ligament injuries on patellofemoral joint
function. Dr. Li also has received a second OREF Grant with Dr. James
Herndon entitled, “ Interosseous Ligament (IOL) Reconstruction in
Forearm Fracture -An in- vitro Experimental Study Using Robotic Technology
”. Dr. Li is highly qualified to carry out the mission of this fine
laboratory.
ORTHOPAEDIC
BIOLOGY AND ONCOLOGY LABORATORIES
The Orthopaedic
Biology and Oncology Laboratory under the direction of Dr. Henry Mankin
has studied the area of normal and osteoarthritic cartilage for many years.
Dr. Mankin explains the Laboratory ’s focus, “ the Orthopaedic
Biology and Oncology Laboratories continue to explore the problems of
the causes and treatment of osteoarthritis. We have an interest in both
the factors that cause cartilage to grow and the degradative cascade that
leads to destruction of the tissue and poorly functioning joints. We are
also continuing to seek factors which may serve as predictors of metastasis
in malignant bone and soft tissue tumors both by biochemical studies and
by flow cytometric analyses of DNA structure and division. ”This
Laboratory is funded through NIH Grants as well as Orthopaedic Research
Education Foundation Grants and a corporate sponsored grant. Dr. Christine
Towle and the investigators in the Laboratory, are studying the effects
of static compression on IL-1 metabolism in cartilage, and the mechanisms
involved in TGF beta effects on aggrecan catabolism. Dr. Towle, reports,
“ There is immense interest in biology-based strategies to interfere
with the loss of articular cartilage. ”In addition, they are investigating
the area of chondoprotective effects of light on photosensitive cartilage,
and intracellular roles for IL-1 in osteoarthritis. Drs. Henry Mankin,
Christine Towle and co-workers should be congratu- lated on their contributions
to the Orthopaedic Research Society meeting.
SARCOMA
MOLECULAR BIOLOGY LABORATORY
The new Sarcoma
Molecular Biology Laboratory, located on Jackson 11, has opened to support
the research efforts of Dr. Francis Hornicek, and Dr. Lawrence Weissbach.
Dr. Hornicek reports, “ the Sarcoma Molecular Biology Laboratory
is part of the biologic section of the MGH Orthopaedic Research Laboratories.
It has been established to investigate new pos- sible agents for treating
cancer and to clarify their mechanism of action ”.
The Orthopaedic Research
Laboratories at MGH have a longstanding interest in cancer research, as
exemplified by the important work on chondrosarcoma metabolism studies
carried out by Dr. Henry Mankin, and tumor suppressor genes in osteosarcoma,
performed by Dr. Mark Gebhardt. The Sarcoma Molecular Biology Laboratory
consolidates different aspects of musculoskeletal tumor research, with
a focus on molecular and cellular aspects of different sarcomas, including
investigation of novel chemotherapeutics, mechanisms of drug resistance,
and antiangiogenesis therapy. Assessment of the in vitro and in vivo potential
of novel antiangiogenic and chemotherapeutic agents on sarcoma cell growth
is being carried out, for certain sarcomas do not respond well to conventional
cancer treatments. The laborator y currently houses two research fellows,
Dr. Hideo Morioka, is exploring the mechanism of action of a novel antiangiogenesis
agent and Dr. Li Shao who is interested in a novel marine-derived chemotherapeutic
agent for sarcomas. Dr. Lei Cai is a techni- cian supporting studies on
the effects of antiangiogenic com- pounds on normal cells. I look for
ward to the many important contributions from this laboratory.
LABORATORY
OF ORTHOPAEDIC BIOCHEMISTRY AND OA THERAPY
Dr. Teresa Morales,
is continuing her important work on the investigation of growth factor
regulations of osteoarthritic cartilage. Dr. Morales, explains, “
the main goal of our studies is to provide fundamental knowledge of selected
areas of the cell biology and biochemistry of cartilage that are likely
to yield fertile soil for the development of approaches and technology
for bioengineering of osteoarthritic tissues into a repair modality ”.
Dr. Morales ’research has been recently supported by the National
Institute on Aging (NIA) and is currently funded by The National Institute
of Arthritis, Musculoskeletal and Skin Diseases (NIAMS) and the National
Arthritis Foundation. The keen areas of interest in this laboratory are
the engineering of chondrocyte migration to dispense into and populate
cartilage so as to promote repair and the investigation into Insulin-like
growth factors binding proteins. She is also working in collaboration
with bioengineer- ing researchers, Drs. Douglas A. Lauffenburger, and
Alan Grodzinsky from MIT. Dr. Morales has been recently named chair of
the Cell Biology Study Section of the National Arthritis Foundation. In
addition, she has also been a member of the Peer Review Council of the
Arthritis Foundation for several years. Dr. Morales had a podium presentation
at the ORS entitled, Insulin-Like Binding Proteins in Fresh Human Cartilage:
Study of Normal and Osteoarthritic Samples, ”and has two new grant
applications with the NIH. In the near future we will be moving this laboratory
to Jackson 12.
BIOMOTION
LABORATORY
The Biomotion
Laboratory is directed by Dr. David Krebs, and is located in Ruth Sleeper
Hall. The Lab investigates the mechanical and neural constraints of human
locomotion. There are two distinct research areas in the Biomotion Laboratory:
Balance/Inner ear Cerebellum problems and Arthritis/DJD. For the former
the Biomotion Laboratory works closely with the Neurology Service. In
collaboration with the Department of Orthopaedics, the Laboratory has
developed an in vivo model of acetabular geometry and wear patterns based
on pressure measurements from a subject with an instrumented femoral athroplasty.
They have also developed MRI techniques 37 that accurately reconstruct
anatomically correct 3D acetubular cartilage thickness. The Biomotion
Laborator y has many interests in common with Orthopaedics. A new study
is underway to study functional practice versus strengthening for knee
arthritis patients and Dr. Krebs says of this collaboration, “ The
Biomotion Lab has enjoyed a strong relationship with our parent Department,
Orthopaedics, since its conception in 1984. Currently more than five attending
Orthopaedists are funded on or working with our research projects. ”Dr.
Krebs and the Laboratory should be congratulated for publishing over 20
research articles throughout the past year. In addition they have three
US Patents pending.
 |
| Frederick
and Joan Brengel shown with Drs. Harris and Mankin |
FREDERICK
AND JOAN BRENGEL LEARNING CENTER
We were saddened
in October by the death of benefactor, Frederick Brengel, a devoted friend
of the MGH. Last year we established through the generosity of the Brengel
Family, The Frederick and Joan Brengel Learning Center. The MGH named
this center in appreciation of their over whelming generosity. Mr. Brengel
was the retired Chairman of Johnson Control Systems, a major manufacturer
of thermostats and temperature monitoring devices. He and his wife resided
in Milwaukee and in Jupiter Island, Florida. I am lucky to have come to
know the Brengel ’s and to experience the depth of their generosity
and their concern for the future of medicine. The endowment of the Brengel
Resource Learning Center is a strong legacy to the Department and the
MGH in furthering the education of orthopaedic residents and fellows.
The Frederick and Joan Brengel Learning Center has been a tremendous new
resource for the residents, fellows, and staff at the MGH.
 |
| Dr.
David Golden utilizing one of the new computer workstations in Frederick
and Joan Brengel Learning Center |
The Center includes
the beautifully renovated Smith-Peterson Library. Volumes housed here
include the traditional material in the Smith-Peterson Library
as well as those from the personal library of Dr. James Herndon and myself.
This extensive library in one of the finest in orthopaedic surgery and
is an extremely important resource in the training program. In addition,
the Smith Resident Education Center as well as the new reading room are
completely renovated and include new workstations, multi-media equipment,
and a place for our new librarian. Finally, we are able to utilize our
newly created and yet unnamed conference room, which includes a state-of-the-art
projection system and other materials, which will serve our staff, residents
and physicians very well.
AOA
ABC TRAVELING FELLOWS
This past year,
in addition to hosting Fellows from the Hellenic Orthopaedic Association,
and The Japanese Orthopaedic Association we had a wonderful time with
the AOA ABC Traveling Fellows. This year ’s Fellows group included:
Jegan Krishan, Evelian Burger, Khalid Mohammed, Grey Giddons, Feral Monsell,
Mike Robinson, and Joahn Witt. They had a broad range of interest from
pediatric orthopaedics to sports medicine. The Fellows were able to present
their research papers to the group and we had a highly interactive didactic
session with them. I would like to thank the members of the faculty and
staff who put a great deal of time and effort into making this a wonderful
visit for the ABC Fellows.
 |
| Piper
Hayden with Santa |
This year we began
a new tradition at the MGH Orthopaedics Department, when we sponsored
a Children ’s Holiday Party for families and friends in a private
party room at The Boston Children ’s Museum. Dr. Shawn Hayden recalls
how the idea for the Holiday Party developed, “ Dr. Rubash was speaking
with several Residents and Fellows during a Clinic Break in the fall and
there was some discussion on how we might make the training experience
more oriented to the growing number of Residents and Fellows with families.
The idea of a Children ’s Holiday Party was presented. Not only was
the initial response positive, but by the time the deadline for RSVP ’s
had arrived it was clear that this event had the makings of a great program
tradition. ”In addition to all the activities and sights that the
Museum offers, the more than seventy attendants were entertained by a
special visit from Santa Claus and one of his elves. The event was a wonderful
time filled with lunch, balloons, ice cream, cake and gifts for the children.
Parent and child reviews alike were stellar. The Residents and Fellows
and their families greatly enjoyed this party and it will become an annual
holiday event at the MGH.
 |
| ABC Traveling Fellows |
Finally on a personal
note my wife, Kimberly, and I have been gradually dealing with the challenges
of turning a new home, new community, and new school district into a positive
and productive family experience. The move to Boston has given us an opportunity
to evaluate carefully the needs and challenges for each of our family
members. My sons, Bradley (age 14) and Stephen (age 12) had a generally
positive year at the Weston Middle School and have been active in school
academic as well athletic activities. In addition, Kristen (age 10) has
enjoyed the Field School in Weston and horseback riding. Kimberly and
I have been trying our best to support our family and develop a new set
of friends and interests in the Boston area. Finally, I look for ward
to seeing many of you at our Annual Alumni Event at the American Academy
of Orthopaedic Surgeons (AAOS) and please join us this year for the Annual
Harvard Orthopaedic Golf Outing.
Links of interest:
|



