|
The excitement surrounding pediatric orthopaedic clinical care, research and education continues at Children’s Hospital Boston. Surprisingly, eleven years have passed since I’ve been the Chief. The staff has more than doubled, and remarkable growth in patient volume continues. Despite this, the collegial academic environment serving as the foundation for education at Children’s is thriving.
Clinical Programs
Our department has ten clinical programs, two of which are distinct divisions. The divisions are Sports Medicine, headed by Lyle Micheli and Spine Surgery, headed by John Emans. The eight clinical programs identified by the department as distinct areas for clinical care and research include trauma, growth, cerebral palsy, myelomeningocele, upper extremity, oncology, and general orthopaedics. By identifying these discrete areas, I believe that we have improved and expanded clinical care as well as research interests. This academic and programmatic subspecialization in pediatric orthopaedics is somewhat at variance with the traditional thought that a pediatric orthopaedic surgeon operated on all areas of the body in an age-defined specialty. As knowledge and technology evolve, I believe that this transition into greater sub-specialization is necessary, yielding tremendous benefits in the clinical, educational, and research environment.
Increase in clinical volume has occurred in many ways. Contraction of small pediatric units in general hospitals in the greater Boston and New England areas has resulted in expand-ed referral for pediatric trauma. In a paper just published this year, I noted that the incidence of supracondylar fractures requiring hospitalization in New England has remained basically unchanged from 1992 to 2002, but there was a four-fold increase in the numbers of Type III supracondylar fractures of the humerus cared for at Children’s. Such trends and volume shifts have a significant impact on our educational environment. In addition to volume shifts, innovation has contributed significantly to our programmatic growth. Examples of this include the titanium rib for chest wall expansion in congenital scoliosis and syndromes of thoracic hypoplasia. The program in treatment of Erb’s palsy with brachial plexus repair appears to have a national following, facilitated by an excellent research program, talented clinicians, as well as the Internet. The Adolescent and Young Adult Hip Team specializes in reconstructive procedures of the hip including periacetabular osteotomy and surgical dislocation and complex femoral osteotomy of the hip in adolescents and young adults. The Advanced Fetal Care Center at Children’s Hospital continues to see an increasing number of pregnant mothers in consultation for babies with congenital defects. Orthopaedics plays a major role in this group in discussion of upper limb deficiencies, spinal deformities and lower extremity congenital deformities, most frequently clubfeet, prior to the birth of the child (Figure 1a & 1b)
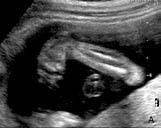 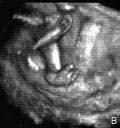
Figure 1A
Fetal Ultrasound of a clubfoot
Figure 1B
3-D fetal ultrasound of a clubfoot
To accommodate the clinical growth, it is necessary to add both new staff and new facilities. Our department now numbers twenty individuals with two being part-time. Over the past year, we have added two orthopaedic surgeons, with Martha Murray joining the staff in early 2004 and Donald Bae in September 2004. In addition to orthopaedic surgeons, we have increased our nurse practitioner staff to five and our nursing support to five, further expanding the clinical program.
A new building is opening as part of the clinical expansion (Figure 2) which will provide eight new operating rooms on the main campus, as well as increase the inpatient bed capacity for surgical services by 30, to 102 beds; there no longer is a distinct orthopaedic floor. We will also add new ICU beds and expand Radiology and Emergency facilities. As you might guess, the clinical expansion of the buildings in the face of packed road-ways around the Longwood Campus presents a major challenge. With this in mind, Children’s bought Waltham Hospital earlier this year and is moving ahead with clinical expansion, providing outpatient consultation as well as surgery in nearly all specialties. Depending on the growth and needs, it is pos-sible that we will open a 15-30 bed unit in Waltham in the next couple of years.

Figure 2
This 11 story tower will house new ICUs, ORs, and surgical beds at Children's Hospital.
With the overall programmatic expansion of Children’s Hospital, one might wonder where orthopaedics falls. At the present time, we use about 25% of operating room hours and do approximately 20% of the total number of cases. Our bed utilization is about constant, based on decreased utilization per case but increased volume. In outpatient programs, our growth target is approximately 4% per year, with an overall volume of ambulatory visits at this time of approximately 58,000. While this growth is desirable in order to expand programs and improve patient care, it must be managed in a way that does not impair the academic culture so important to us.
Academic Programs
  Resident and fellow education remain central to our mission. We have increased the number of Harvard residents from 10 per year to 12 per year, (Figure 3, Figure 4) which will result in an additional resident here at Children’s for their 6-month third-year rotation. With the 80-hour work week and the change to a night float system, this will provide us a level number of residents providing patient care. Three years ago, we increased the number of pediatric orthopaedic fellows from 2 to 3 and have added a full-time hand fellow as part of the Brigham and Women’s/Children’s Hospital hand program. We increased our tumor fellow presence as well. With the number of individuals involved in patient care, it is mandatory that cross coverage be provided accurately and hand-off in patient care be done seamlessly. I believe that the computer systems which are developing and the culture support this process but it requires diligence and management in order to effect these changes. In the absence of a chief resident at our institution, it has required increased efforts of junior faculty in managing resident schedules, coordinating resident conferences and in general, managing the educational program. We solicit feedback from the residents on a regular basis and continue to change the program in response to their constructive criticism. Our conference schedule remains similar to what it has been in the past, with 6:30AM conferences each morning including fracture, basic science, pediatric orthopaedics, indications conference and fellows’ conference. We have added an every-other-week basic science conference on Friday afternoon which has been an outstanding addition to the Longwood musculoskeletal research environment. In November 2004, we hosted Professor Reinhold Ganz for the 18th David Grice lectureship. This was held in conjunction with a reunion for past residents and fellows which we try to do every 3-5 years (Figure 5, Figure 6). Resident and fellow education remain central to our mission. We have increased the number of Harvard residents from 10 per year to 12 per year, (Figure 3, Figure 4) which will result in an additional resident here at Children’s for their 6-month third-year rotation. With the 80-hour work week and the change to a night float system, this will provide us a level number of residents providing patient care. Three years ago, we increased the number of pediatric orthopaedic fellows from 2 to 3 and have added a full-time hand fellow as part of the Brigham and Women’s/Children’s Hospital hand program. We increased our tumor fellow presence as well. With the number of individuals involved in patient care, it is mandatory that cross coverage be provided accurately and hand-off in patient care be done seamlessly. I believe that the computer systems which are developing and the culture support this process but it requires diligence and management in order to effect these changes. In the absence of a chief resident at our institution, it has required increased efforts of junior faculty in managing resident schedules, coordinating resident conferences and in general, managing the educational program. We solicit feedback from the residents on a regular basis and continue to change the program in response to their constructive criticism. Our conference schedule remains similar to what it has been in the past, with 6:30AM conferences each morning including fracture, basic science, pediatric orthopaedics, indications conference and fellows’ conference. We have added an every-other-week basic science conference on Friday afternoon which has been an outstanding addition to the Longwood musculoskeletal research environment. In November 2004, we hosted Professor Reinhold Ganz for the 18th David Grice lectureship. This was held in conjunction with a reunion for past residents and fellows which we try to do every 3-5 years (Figure 5, Figure 6).
 
Research
From a research perspective, we have had another rather successful year. For the second year in a row, one of our staff members has won a Kappa Delta Award from ORS/AAOS. This year Min Kocher received this award for clinical research based on the study of septic arthritis in children and the development of a clinical practice guideline in this area. Last year, Brian Snyder received the Kappa Delta Award for research on bone strength in metastatic disease, delineating methods of predicting fracture risk.
Signficant research programs are underway in the study of brachial plexus repair and orthopaedic reconstruction in cases of Erb’s palsy by Peter Waters. Young Jo Kim is continuing to develop methods for determining articular cartilage changes in hip dysplasia and the response of articular cartilage to acetabular reorientation. Martha Murray is supported by the OREF, the National Football League and NIH in her work on augmentation of intra-articular healing involving both the ACL and menisci. Min Kocher received the Ann G. Kuo Award from the Pediatric Orthopaedic Society of North America. Min heads up our Clinical Effective Unit which now has 5 research assistants and is increasing its research productivity as well as funding.
On the basic science research area, we have been conducting a search for an additional professor with a combined appointment in Genetics and Orthopaedics. Hopefully, we will complete the search this summer. The continued work in the lab under the direction of Drs Hauschka and Glimcher remains productive with significant publications involving bone structure and control of bone deposition and resorption. Use of MRI in determining bone density is an area of innovation under the direction of Mel Glimcher.
Staff Development
 Over the past several years, John Hall (Figure 7) has continued to see patients on Thursday mornings and participate in conferences. With his 80th birthday this spring, John decided to totally stop seeing patients at the end of the academic year. He is an active contributor at our morning conferences on Thursday and Friday mornings. I predict that even in his clinical retirement, his presence in morning conferences will be felt. He will certainly continue to impact resident, fellow and staff education. Congratulations to Dr Hall for a wonderful career and thanks from all of us who have benefited from our association with him. Over the past several years, John Hall (Figure 7) has continued to see patients on Thursday mornings and participate in conferences. With his 80th birthday this spring, John decided to totally stop seeing patients at the end of the academic year. He is an active contributor at our morning conferences on Thursday and Friday mornings. I predict that even in his clinical retirement, his presence in morning conferences will be felt. He will certainly continue to impact resident, fellow and staff education. Congratulations to Dr Hall for a wonderful career and thanks from all of us who have benefited from our association with him.
Donald Bae and Martha Murray joined the staff in 2004. Martha is now about 75% committed to basic science research; she is supported by the NIH under a K award as well as a number of other funding agencies. Peter Gerbino is active in the Medical Education Committee of the American College of Sports Medicine, as well as having a significant role in teaching in the Sports Medicine fellowship and the primary care Sports Medicine fellowship, both of which are now ACGME-approved. Lyle Micheli has been elected to the Athletic Trainers of Massachusetts Hall of Fame. He also has been promoted to Professor at Harvard Medical School. In his honor, a Children’s chair in Sports Medicine research has been funded by several grateful families. The formal announcement of this chair will be coming in the next several months. Min Kocher is active as director of our clinical research unit and has been named, as a junior member, to the Board of the Pediatric Orthopaedic Society of North America. Brian Snyder is continuing as the Director of the Orthopaedic Biomechanics Laboratory at Beth Israel Deaconess Medical Center, in addition to his clinical responsibilities in the Cerebral Palsy Clinic here.
On a personal note, I have completed my 9 years on the Board of the Pediatric Orthopaedic Society of North America and leave the presidential line behind. I have just been appointed to the American Board of Orthopaedic Surgery. I am president of the Physicians’ Organization at Children’s Hospital, Boston and active on the Board of Trustees of the hospital. Within the medical school, I am on the Executive Committee of the Medical Education Reform, ensuring that we continue to produce committed doctors and have a curriculum that supports this in its broadest aspects.
Our management team for the Children’s Orthopaedic Surgery Foundation includes Jim Cote as the Department Administrator, Dean Bauer as our Financial Manager, Susanne Ellard as our Program Administrator, and my assistant, Kathryn MacDonald. Peter Waters was named Associate Chief of the Department last year and is doing an outstanding job with primary responsibilities in the ambulatory area. Peter has also just completed the process of professorial appointment at Harvard Medical School and the appointment will become official in the very near future.
Harvard residents continue to view Children’s as a very positive academic experience. Each morning conference provides a learning experience supported by staff focusing on an area of pediatric orthopaedics. While there is a national short-age of pediatric orthopaedic surgeons, we continue to see our residents enter pediatric orthopaedics in significant numbers; hopefully this will continue.
Links of interest:
|

